Since its inception in 2001, RCH1000 has provided vital support to research that is revolutionising the way sick children are cared for at The Royal Children’s Hospital (RCH). Read on for the significant projects RCH1000 has supported over 20 years.
2004
The Australia & New Zealand Children’s Heart Research Centre at the RCH
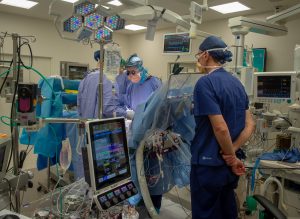
Though commonly thought of as an older person’s condition, heart disease is a serious issue for children too. Nearly 10 in every 1,000 babies born will be diagnosed with congenital heart disease, a term describing heart abnormalities discovered in utero or at birth. Though less common, some children are affected by acquired heart disease in later childhood.
To better understand the causes of paediatric heart disease and how best to treat it, RCH100 supported the establishment of The Australia & New Zealand Children’s Heart Research Centre at the RCH. Built adjacent to the old hospital, the Centre employed a team of full time researchers who developed new treatments for children who could not have been treated a decade prior.
In addition to their work aiming to understand congenital and acquired heart disease in children, research also extended to the examination of foetal circulation, the effects of the repair of congenital heart disease on the developing brain in early childhood and the effects of premature birth on cardiovascular health in young adults. The team also worked on the development of novel techniques to examine these complex conditions.
2007
The Paediatric Stroke Neuroscience Research Facility at the RCH
 Another condition often thought to affect the elderly, childhood stroke occurs more often than you think. Each year, approximately two children in every 100,000 will suffer a stroke. One of the top 10 causes of death in childhood, stroke also had the highest mortality rate in the first 12 months of life. Of the survivors, 50-85 per cent will have long term health concerns including seizures, physical and/or development disability, and speech impediments.
Another condition often thought to affect the elderly, childhood stroke occurs more often than you think. Each year, approximately two children in every 100,000 will suffer a stroke. One of the top 10 causes of death in childhood, stroke also had the highest mortality rate in the first 12 months of life. Of the survivors, 50-85 per cent will have long term health concerns including seizures, physical and/or development disability, and speech impediments.
The Paediatric Stroke Neuroscience Research Facility helped the hospital expand its care and research programs for children affected by stroke and epilepsy. As part of this, the RCH joined the International Paediatric Stroke Consortium to collaborate with colleagues in the US, Canada and the United Kingdom. By entering patient data into an International Childhood Stroke Registry, the RCH team assisted with research studies including validation of a paediatric stroke scale and multicentre randomised controlled preventative treatment trials.
2010
Developmental and Functional Brain Imaging Research Laboratory
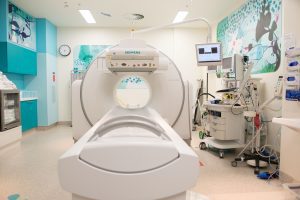 Advances in brain imaging over the last two decades, particularly magnetic resonance imaging (MRI), have led to significant improvements in the diagnosis and treatment of neurological disorders in children. Not only does MRI detect and characterise underlying brain lesions, it can provide important information about brain functions, pathways, networks, circulation, chemistry and metabolism. When combined with metabolic data from positron emission tomography (PET) and electrical data from electroencephalography (EEG), even more detailed images of brain structures and processes can be generated and manipulated, to better inform diagnosis and treatment.
Advances in brain imaging over the last two decades, particularly magnetic resonance imaging (MRI), have led to significant improvements in the diagnosis and treatment of neurological disorders in children. Not only does MRI detect and characterise underlying brain lesions, it can provide important information about brain functions, pathways, networks, circulation, chemistry and metabolism. When combined with metabolic data from positron emission tomography (PET) and electrical data from electroencephalography (EEG), even more detailed images of brain structures and processes can be generated and manipulated, to better inform diagnosis and treatment.
At the RCH, the benefits of this neuroimaging revolution have been most notable in the areas of epilepsy, brain tumours, stroke, multiple sclerosis and brain malformations, areas in which the RCH is recognised nationally and internationally for its excellence in neuroimaging and treatment.
With the employment of two research officers for the MCRI Developmental Imaging Group, MCRI was able to increase the Developmental and Functional Brain Imaging Research Laboratory’s capacity. Between them, the research officers processed brain imaging data in over 400 children, generating images that have been vital for management of seizures, tumours and strokes. Furthermore, during the period of RCH1000 funding, 260 epilepsy surgery operations were undertaken at the RCH, each drawing on some aspect of advanced neuroimaging.
Brain scanning and processing performed by the two neuroimaging scientists include combining PET scans of brain metabolism and MRI scans of brain structure to define brain regions giving rise to seizures in children with epilepsy, preparing 3D brain surface maps from MRI scans to reveal safe neurosurgical access to lesions, simultaneous EEG recording and functional MRI imaging of brain activity in the scanner to study seizure networks in epilepsy, functional MRI localisation of normal language and motor functions in the brain, nerve fibre tracking of visual, sensorimotor and language pathways, generating images of brain blood flow in children with stroke, and functional MRI of seizures recorded in the MRI scanner.
The Developmental Imaging Group team has developed and implement advanced brain imaging and image analysis methods, scanning thousands of children per year and completing over 175 research projects.
2012
Childhood Origins of Heart Disease

It’s a well-known phenomenon that many acquired diseases in adults have their origins in childhood. Common problems like high blood pressure and obesity begin to occur through bad habits or possibly through illnesses these children have suffered. The RCH Cardiology team believe that these other childhood conditions have an effect on the health of blood vessels and the heart, and investigated this theory.
Diseases characterised by inflammation like obesity, inflammatory bowel disease and arthritis are known to increase the incidence of heart attacks and strokes. However, it’s yet to be determined whether the diseases or their treatment cause the acceleration of cardiovascular problems.
There are a number of ways to detect early abnormal changes in the structure and function of blood vessels which cause heart disease. If these changes are proven to be present in young people with chronic illness, it would allow for earlier identification of at-risk individuals and potentially earlier treatment or preventative measures.
Several research studies play an important part in this project:
Barwon Infant Study
Recruiting more than 1,000 children, this study assessed them from pregnancy to the age of four. The study showed that faster weight gain in early infancy due to an excessive intake of calories is associated with thicker blood vessel walls, an indicator of increased risk for future cardiac issues.
Longitudinal Study of Australian Children
This study assessed over 1,500 children across Australia since birth, making detailed health and lifestyle measurements including vascular and lung function measurements.
Non-Invasive Measure of Blood Pressure Study
This study worked to determine an age appropriate measurement of central aortic pressure, or pressure in the part of the aorta closest to the pumping chamber of the heart, through the use of a standard blood pressure cuff.
Studying the Effects of HIV on the Heart
In a collaboration with colleagues in Jakarta, RCH Cardiology studied the effects of HIV and the associated drug therapy on children with the virus. Findings showed that HIV makes the heart more prone to abnormal heart rhythms and reduced function.
Pluripotent Stem Cells
Through a new process called pluripotency, RCH Cardiology grew heart muscle and vascular stem cells from patients with pulmonary hypertension, aiming to use the stem cells to heal damaged tissues.
2014-2021
Harmonising Age Pathology Parameters in Kids (HAPPI Kids) research study I and II
 HAPPI Kids I
HAPPI Kids I
Blood tests are vital in diagnosing whether a person is sick, monitoring the progress of their illness and treatment, or confirming if they are, medically speaking, ‘normal’. Normal is considered as a reading in the range where 95 per cent of the population lie when in good health and is what blood tests are measured against. However, the normal range changes with age and what is a normal reading for an adult is very different to that of a child. The HAPPI Kids I study, funded by RCH1000 addressed this dilemma by collecting blood samples from ‘normal’ healthy babies and children from birth to 18 years old and used this data to build a new paediatric centred database. Researchers can now measure the blood tests of sick children against data that is more relevant to what is normal for their age. This research is a significant step forward in understanding the clinical use of these tests in children not only at the RCH, but in the wider medical community in Australia and abroad.
HAPPI Kids II
Building on the vital data gathered in HAPPI Kids I, the second stage of this study is expanded to support the diagnoses, monitoring and treatment of more complex blood conditions. Using the same methods as HAPPI Kids I, highly trained pathology collectors worked in collaboration with The Royal Women’s, Sunshine and Northern Hospitals to obtain samples from ‘healthy’ newborn and prematurely born babies to those aged up to 18 who visited hospital for minor day surgery. The blood samples underwent three tests; an immunology cellular test (used in the diagnosis and management of immunity deficiencies), a telomere length test (telomeres are caps at the end of each strand of DNA, measuring telomere length is important for the diagnosis of blood cell and bone marrow diseases), and a platelet flow cytometry test (which helps with the diagnosis of bleeding disorders).
COVID-19 research
Researchers from the RCH, University of Melbourne Department of Paediatrics and the Murdoch Children’s Research Institute are collaborating with teams globally to understand why children are less likely to display signs of COVID-19, and the key is in their blood. The data from the HAPPI Kids studies has been vital to understanding the impact of COVID-19 in children as it provides an accurate reference point for comparison. The results from these studies will be extremely significant in helping to understand the impact of COVID-19 on blood clotting both in children and adults right around the world. This will then help clinicians to decipher which treatments to use to combat symptoms of COVID-19.
2022 – now
Melbourne Children’s Campus Mental Health Strategy
 Each year thousands of children come through the doors of the RCH with physical health problems, but many have mental health problems too. Some children are particularly at risk of developing mental health problems like those with a chronic medical condition, refugee children, children living in foster care, patients from the Gender Service, Indigenous children and those from linguistically or culturally diverse backgrounds. Led by Professor Harriet Hiscock, Director of Research at the Centre for Community Child Health, this innovative project aims to provide a uniform and evidence-based approach to mental health prevention, care and advocacy for all patients and their families across the RCH campus. RCH1000 is supporting the research arm of the Mental Health Strategy, funding a professorial lead in research and a senior implementation scientist to make sure the research conducted generates changes that will flow on into practice and care for patients, their families and the broader community.
Each year thousands of children come through the doors of the RCH with physical health problems, but many have mental health problems too. Some children are particularly at risk of developing mental health problems like those with a chronic medical condition, refugee children, children living in foster care, patients from the Gender Service, Indigenous children and those from linguistically or culturally diverse backgrounds. Led by Professor Harriet Hiscock, Director of Research at the Centre for Community Child Health, this innovative project aims to provide a uniform and evidence-based approach to mental health prevention, care and advocacy for all patients and their families across the RCH campus. RCH1000 is supporting the research arm of the Mental Health Strategy, funding a professorial lead in research and a senior implementation scientist to make sure the research conducted generates changes that will flow on into practice and care for patients, their families and the broader community.