Originally published in the Herald Sun, 30 March 2021
Words: Brigid O’Connell
Photo: David Caird
For the 200 young people — some in their first week of life — who enter the Royal Children’s Hospital’s (RCH) Children’s Cancer Centre each year, everything is thrown at outsmarting the rogue cells that have hijacked their childhood.
“We cure somewhere between 80 to 85 per cent of children who walk through the door. Not extend life, which is the focus of care for adult medicine; we cure,” said paediatric oncologist Jordan Hansford.
“The thing we do well is we have international collaborative projects for rare disease so our outcomes are outstanding.”
But it is a hard road to walk.
Cancer treatment is long, intense and isolating, not just for the patient but their family, too. It typically leads to families living apart for weeks or months on end; parents play tag team to spend the night on the couch by their child’s side.
And the stress doesn’t ease once they are at home for brief periods between rounds of chemotherapy. A spike in fever can be life threatening, so patients must get to the emergency department within the hour. Battered immune systems mean families are forced to live in COVID-style lockdown for months or years, to keep their child safe.
It’s a precarious way to live.
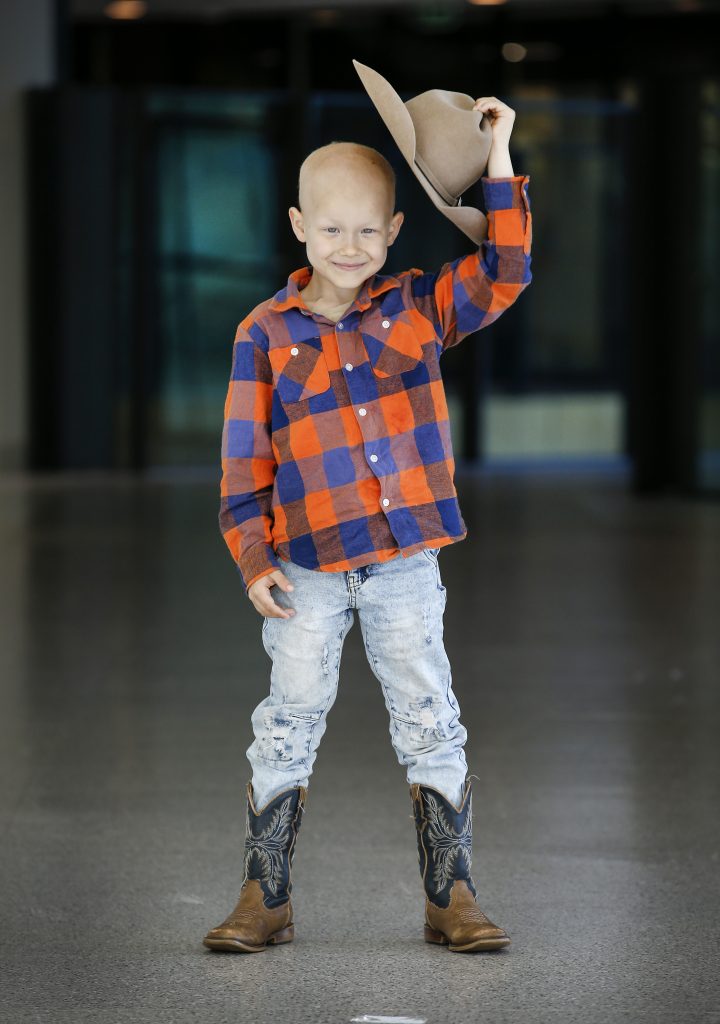
Eddie Biemans, age seven, from Alberton has a rare cancer condition called Hepatoblastoma likes to wear his cowboy clothes to oncology treatment at the RCH. Picture: David Caird.
But for families like Eddie Biemans’s, they take strength and solace in the resilient way their child endures the treatment, and the dedication of their medical team.
Sammy and Hayden Biemans were forced to quit their jobs, leave their cattle farm in the state’s far east and find a temporary home for the family in Melbourne, after their seven-year-old was diagnosed with liver cancer in September.
“It’s a really surreal situation. You have to put your blinkers on, like horses do, and have the vision of getting out of it and dealing with everything else later,” Ms Biemans said.
Despite the cancer initially spreading to Eddie’s lungs, high-dose chemotherapy cleared it. The Alberton boy had surgery two days before Christmas to remove the tumour and most of his liver and gallbladder.
With Eddie able to ring the gold bell in the oncology ward — a hospital tradition to signify the end of treatment — the family will continue to travel to the RCH for the next two years for monthly blood tests and regular scans.
“It’s hard for people to understand that every admission into hospital, it’s blood tests, it’s scans, the kids having to deal with random people coming into their room invading their personal space,” Ms Biemans said.
“But he’s been able to make connections with play therapists and the education team — people who weren’t coming to poke and prod him — so it meant he had things he looked forward to.”
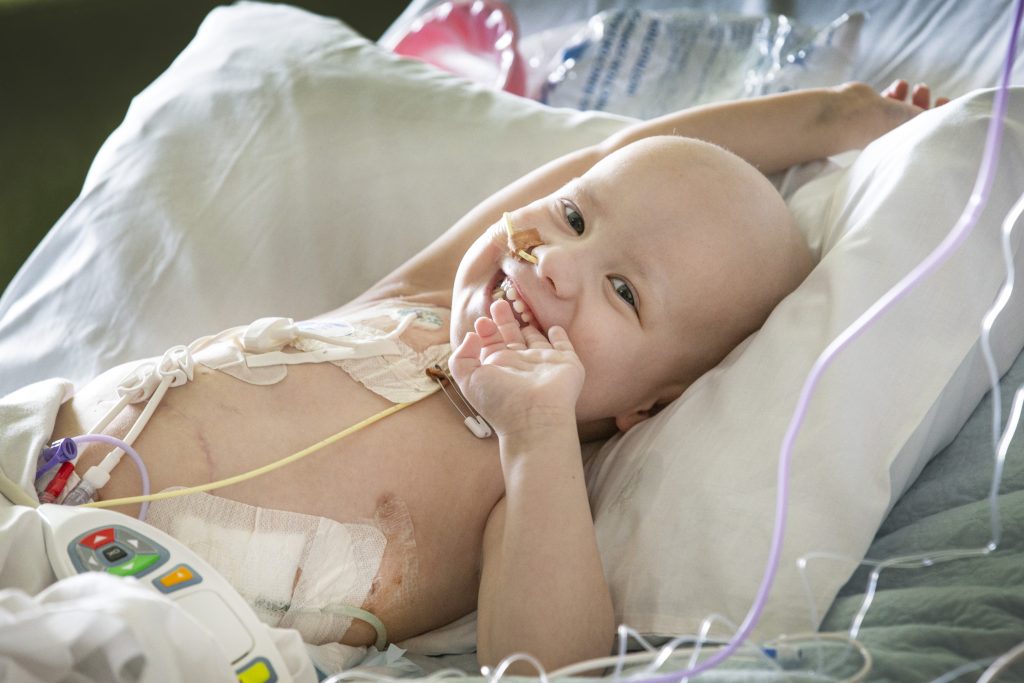
Cancer patient Oli Pluelkhahn, age three. Picture: David Caird
All the tools in the oncologist’s kit are being thrown at three-year-old Oli Pluelkhahn after he was diagnosed with a rare and aggressive neuroblastoma in September.
He has undergone chemotherapy and a 10-hour surgery, and faces more chemotherapy, a stem cell transplant, radiation and immunotherapy, which will start as soon as he recovers from treatment complications.
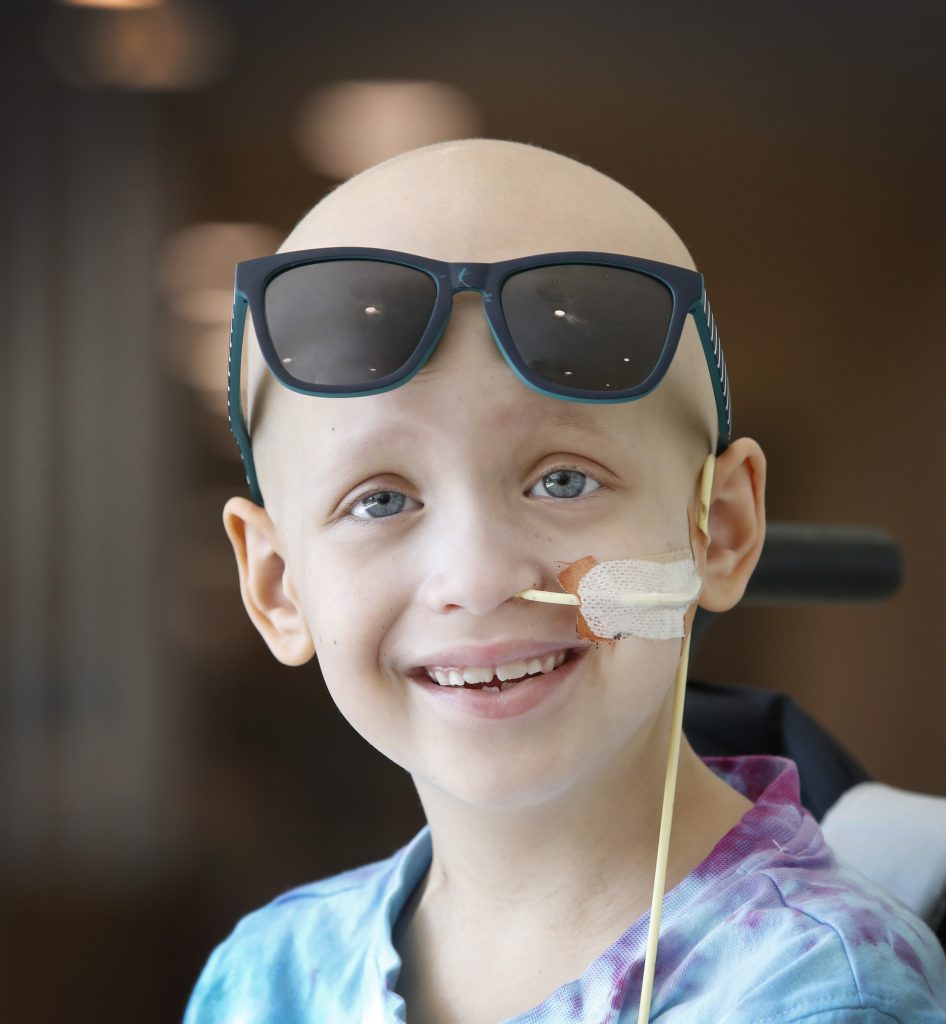
Nolan Hiotakis, age seven, being treated for brain cancer. Picture: David Caird
Further down the ward, Nolan Hiotakis, 7, is experiencing his own side effects from chemotherapy. The treatment for his brain tumour has made him light-sensitive, meaning he must don shades when chilling out.
Dr Hansford, who also runs the oncology clinical trials unit, said the centre relied on donations to support their mission statement of getting each child access to the most promising treatment.
“Our model of care is such that every child who walks through the door and needs treatment, our goal is to enrol them on a clinical trial,” he said.
“The only way we get success with these children is through our collaborative clinical trials. Much of our money to staff and operate this program is soft, it’s not ongoing.
“We’re reliant on the goodness of public will through the Good Friday Appeal and through other charities and competitive grants, to help run our facility.”