Originally published in the Herald Sun, 2 April 2021
Words: Brigid O’Connell
Photo: David Caird
Since a rare kidney condition forced his entrance into the world three months early, it has been all hands on deck to save Sonny Grossman.
1 April 2021 was supposed to be the first day Kim Spencer and Danny Grossman would wake up with their newborn. Instead, Sonny has spent his entire life in hospital, where specialists at The Royal Children’s Hospital (RCH) have performed a delicate balancing act to boost his kidneys.
It was a textbook pregnancy up until about 20 weeks. But then fluid started to collect around Sonny.
The build-up was so big that Kim was generally measuring eight weeks ahead in the second trimester. But by 28 weeks her abdomen was the size of a full-term pregnancy.
“I’ve been pregnant before so I knew I would get big, but not that big,” she said.
“Usually the second trimester is much easier, but this second trimester was not kind.”
An amniocentesis was performed, a procedure where a sample was taken of the fluid around the baby, but that had not detected the cause.
At each scan the fluid kept building. Little did they know Sonny’s kidneys were unable to retain any fluid.

Sonny is gently kissed by his mother Kimberley in NICU. Picture: David Caird
When Kim reached 28 weeks and the fluid build-up was almost unbearable, doctors decided to drain some of it. But it is a highly risky procedure, as entering the amnionic sac can trigger premature labour.
In preparation, Kim was given steroids as a last-ditch effort to protect the baby’s lungs and brain if he did arrive early.
On 8 January they drained 1.4 litres, but the procedure had to be stopped when Sonny became distressed.
Three days later they tried again, and took out 1.6 litres.
“At that point we started to think something is not right. They can’t be for no reason,” she said.
After a few hours of monitoring on the ward, the couple then went downstairs for coffee. Kim collapsed in pain outside the cafe.
“I knew what that pain was straight away. It was my second child,” she said.
“I was pretty terrified in that moment. You know pre-term labour is a risk. But you never think it’s going to be you.”
On 11 January, Sonny arrived weighing 1.15kg, at 28 weeks and four days gestation.
In the first few days of Sonny’s life it became clear his kidneys were causing him problems, and he was transferred to the RCH’s neonatal intensive care ward for the specialist care of the renal team.
Sonny was accepted on to a clinical trial once there, comparing the effectiveness of rapid genetic testing for critically ill bubs.
Neonatologist Ruth Armstrong said the test confirmed he had a rare genetic condition called Bartter syndrome.
“The kidneys filter water, get rid of all the stuff you don’t need, and keep hold of the stuff you do need. Because of his generic alteration, his kidneys are less able to hold on to water, and the water then is more able to freely pass through,” Dr Armstrong said.
“This can be life-threatening, particularly if it goes unrecognised. Babies can become very dehydrated very quickly. They can lose thousands of mils of fluid per kilogram of their body weight a day from their urine.”
It was initially a tricky balance to get his fluid needs right.
“He needed an awful lot of fluid poured into him in order to keep up with his urine output,” she said.
“We started him on some medication with the hope it would reduce his urine output. That has worked, along with growing up a little bit. He’s still needing lots of fluid to keep him hydrated. But he’s managing to take most of that now, orally.
“Watching him take a bottle the other day was a real joy to see.”
The Victorian public also played a part in Sonny’s care. He spent most of the first part of his stay living in one of the infant radiant warmer cots, which were bought through money raised from the Good Friday Appeal.
With a convertible roof and open sides, the cot allows his medical team ready access to ill newborns, without having to move them from their beds.
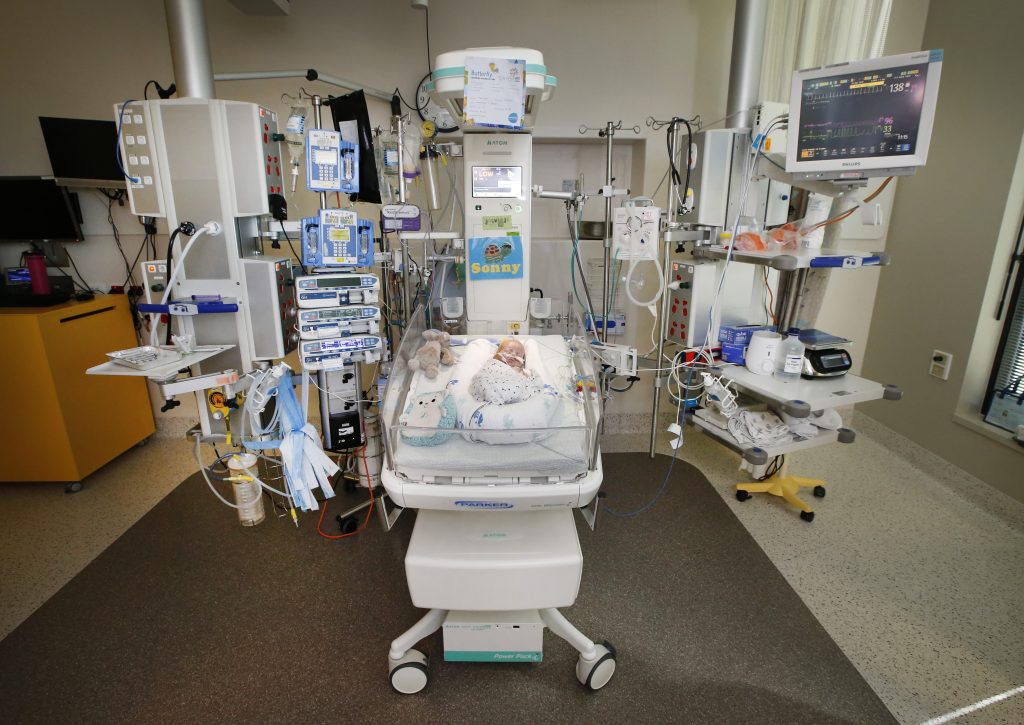
Sonny in the infant radiant warmer funded by the Good Friday Appeal. Picture: David Caird
For Sonny this has meant six lumbar punctures to diagnose infections, and his daily weigh-ins could be done with less stress.
The beds also give parents better access to the tiny children, some who are barely bigger than soft drink cans, for the all-important tender touch and talk with their kids.
“Ultimately the baby is what we’re all there for, but we need to support the family. They need to be able to bond with their very sick baby, and the baby needs to be able to bond with them,” Dr Armstrong said.
“We do know that having parents close by, having cuddles with your mum and dad, having them sing to you or talk to you, or stroke your hand, whatever a baby is able to tolerate, we know that helps them to settle down.
“Their heart rate settles down, their breathing settles down.”
Sonny, who was due to be born yesterday on 1 April , needs to gain more weight on top of his current 2.5kg and confidently take more feeds, before he can look to go home — which is likely to still be a few weeks away.
“It’s such a strange situation to have a 12-week-old baby and not know what they do at night time,” Mr Grossman said.
“That’s why we’re desperate to get him here so we can have a normal family life.”
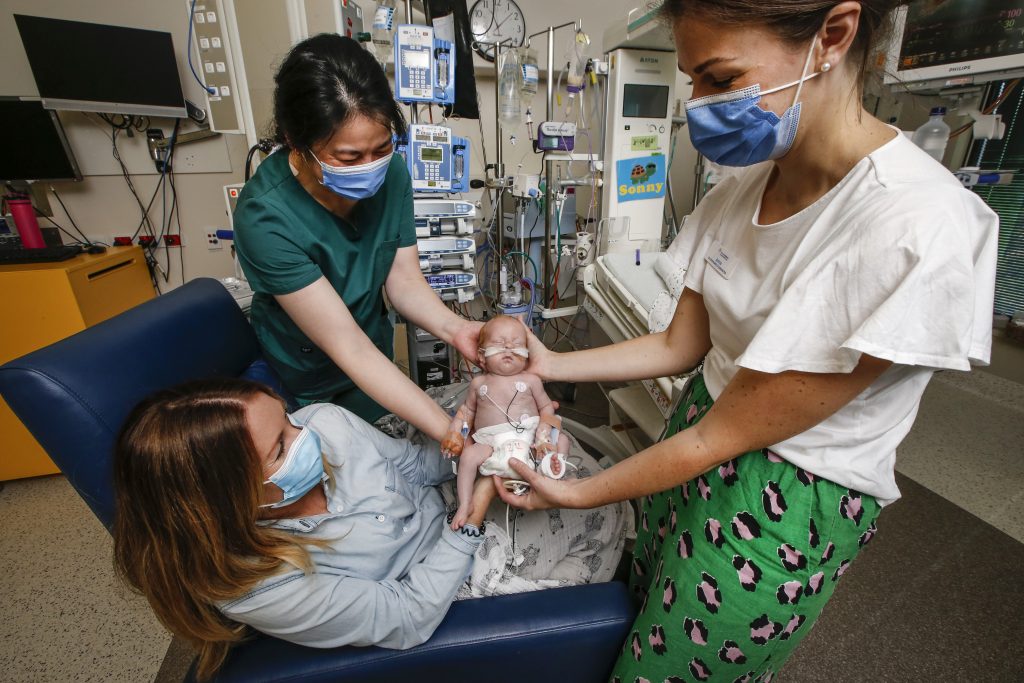
Sonny is moved to his mum Kimberley for a cuddle. Picture: David Caird
Big brother Ethan, who has not yet met his beloved baby in the flesh because of COVID restrictions, must contend with Baby Chat — a virtual health initiative of the hospital that allows sick newborns the chance to hear the voices of their parents and siblings — for a little longer.
Sonny will need continued help with getting enough fluid, which could mean a feeding tube through his nose or directly into his stomach.
He will be watched closely by the RCH renal team over his entire childhood to ensure his kidneys are coping with the challenge.
But in the longer term the hope is that he will simply be able to manage his condition by drinking enough himself.
“A clinician told me that this condition is what we make of it. If we’re not bothered by it then he won’t be. That really stuck with me,” Ms Spencer said.
“I don’t want him to be treated any different to any other child.
“I just want him to learn to live with it and manage it, so he can do whatever he wants to in life.”
Support patient care at the RCH
