To look at five year old Maxwell today, playing at home with his brothers, it’s hard to imagine it is the same sick boy who was once given only a 10 per cent chance of survival in his long battle with leukaemia at The Royal Children’s Hospital (RCH).
When Maxwell was not yet two years old, his mother Victoria knew that something wasn’t right.
“He just wasn’t himself,” Victoria said. “He was normally happy and full of energy. But this time he was tired, pale and running a temperature.”
After feeling Maxwell’s swollen stomach and glands, and taking a blood test, the doctor confirmed that Maxwell had leukaemia.
Victoria was devastated. “My mind automatically jumped to the worst possible outcome. “I remember letting out a guttural cry…it’s like the wind was knocked out of me. I just didn’t expect it,” she said.
Maxwell was quickly taken to the RCH, where he met Dr Diane Hanna, who would become his oncologist, and started treatment at the RCH Children’s Cancer Centre (CCC).
Leukaemia is the most common cancer in children, and thankfully, these days, 85 to 90 per cent of children are cured with standard chemotherapy alone. However, there are a small percentage of children who don’t respond to treatment and, unfortunately, Maxwell was in that group.
After two years of chemotherapy, he hadn’t really improved. Then, a new treatment trial offered hope, but also didn’t work.
“We felt deflated,” remembers Victoria. “And that’s when it hit us. ‘This one didn’t work. Will there be one that does work’?”
The dreadful possibility that there would be no more treatments to try was terrifying for Victoria.
“I remember making notes on my phone to capture different things that Maxwell would say, and different things that were special with him, in case I needed something to help me remember those things if he wasn’t around to say or do them anymore. And I made sure I took so many photos.”
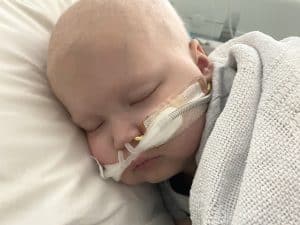
The dedicated staff at the CCC, including Dr Hanna, didn’t give up. There was one more option – a bone marrow transplant.
“I sat the family down and I said, ‘There’s a 10 per cent chance Maxwell will be alive in a year. I’m more sure than not that he’ll relapse. I’m worried he may die from infection before then’. We had palliative care involved at the bone marrow transplant consent discussion.”
“The family knew that this was going to be really tough, and that he might not survive, but they also knew that without it, it was certain death,” said Dr Hanna.
The best donors tend to be siblings, but there is only a one in four chance of a match. It turned out, Maxwell’s older brother Ethan was a match.
Ethan was only six-years-old, so Victoria faced the tricky task of having to explain a bone marrow donation to him in a way he would understand.
“We were very honest with him,” said Victoria. “We said, ‘Your brother is very, very sick and he needs something that’s very special inside your body, and we need to put it into Maxwell’s body to help him fight the disease’. And Ethan was proud to do it.”
Dr Hanna knew Maxwell’s infections wouldn’t go away without a new immune system.
“We needed the transplant and the new stem cells to kick in to help fight these infections. In such a short life, Maxwell had already been through quite a lot. So, if this transplant didn’t work, it would have been really difficult to take him to a second transplant with good success. There was a lot of hope riding on this. We had one chance; we had to do it right. So yeah, he’s our miracle. He’s our Hail Mary transplant,” she said.
The transplant went ahead, and after an agonising wait, Victoria and her husband Jason got the news they were desperately hoping for: the transplant was a success.
Now, Maxwell and Ethan spend their time kicking the footy together at home with their little brother, William.
“I was just glad that he got better and I basically saved his life. I’m a hero,” said Ethan.

From left: William, Maxwell, Ethan and Victoria at home.
The RCH provides world class treatment in a world class facility, but children need even more than outstanding medical care to survive and to thrive.
Maxwell’s treatment started at an age when children are growing fast and normally on a rapid learning curve. Even if he got well, he was at risk of falling behind or suffering from the psychological impacts of his illness.
Thankfully, the RCH is able to provide a comprehensive approach to the care of children who are hospitalised so often, or for so long.
For example, the RCH ‘CARES (4 Kids): Cancer Allied Health Resources, Education and Supportive Care’ program funded by the RCH Foundation ensures children continue grow and learn during their hospital stay.
This includes play and art therapy, which not only provide an important distraction from pain, but also stimulate brain development and fine motor skills.

“Art therapy can be used as an effective modality for self-expression, self-regulation and for processing the experiences of hospital and illness through a creative form. It allows choice and control for patients in a situation in which they have minimal control. Art making can be a starting point for art play, with the art therapist opening up the possibility of endless creative opportunities. Maintaining relationships with family and friends at home is another key aim of art therapy for patients having a bone marrow transplant, creating work for family members or art packs for siblings or caregivers to join in from home,” said Matilda Dawson, Art Therapist at the RCH.
There’s one term Victoria uses to describe how they were treated at the RCH: like family.
“The RCH team are like family because you’re in there, you are living in the hospital. And the nurses that come in and out of the room every day, they’re like family too. You talk to them, and you cry to them. You talk to them about silly things, and you talk to them about the serious things. Amazing doesn’t cut it.”
Maxwell is now at school and is able to get involved with fun things like other kids his age.
“When Maxwell goes to birthday parties, when he does Auskick, when he does the normal things, that’s when I get really emotional because I’m so grateful that he’s here to do it,” said Victoria.
“Having Ethan as a donor for his stem cells, we owe him. But the hospital going ahead with the transplant and not treating him as a number, but treating him as a person instead, we owe them everything. Maxwell wouldn’t be here if it wasn’t for them,” she added.